SUMMARY
Metabolic syndrome is made up of a cluster of conditions including obesity, impaired insulin sensitivity, hypertension, and altered lipid profile. These conditions are also considered as risk factors for type 2 diabetes and cardiovascular disease. The occurrence of these conditions is on the rise worldwide despite the increasing number of drugs used. There is evidence from the literature indicating that intervention with low carbohydrate diets, including the paleolithic diet, may be beneficial in the metabolic syndrome. Except for one study with the paleolithic diet, these investigations are short in duration. Another limitation is that they do not give clues on how to deal with medications patients are treated with. Third, in these studies, the paleolithic diet did not produce ketosis which may limit the clinical effectiveness. Here we present a case of a patient with metabolic syndrome and excessively medicated. The patient shifted toward the paleolithic ketogenic diet and was able to discontinue medication, lost weight, and her glucose parameters markedly improved. Her hypertension normalized. Currently, she is on the diet for 22 months and shows good adherence as also confirmed by laboratory tests. She is free of symptoms and no side effects emerged. Previously we reported cases with epilepsy and type 1 diabetes successfully treated with the same diet. We suggest that a dietary intervention with the paleolithic ketogenic diet may be a simple, feasible, and cost-effective method in some forms of chronic disorders in highly motivated patients.
ABSTRACT
Introduction:
Metabolic syndrome is a major public health problem affecting at least 20 percent of the world’s adult population. Components of the metabolic syndrome include obesity, impaired glucose metabolism, hypertension, and altered lipid profile. Currently, medical treatment relies on drugs. A major problem is that patients with long-standing diseases are excessively medicated because of an increase in the number of symptoms over time. A few clinical studies indicate that low-carbohydrate diets, including the paleolithic as well as the ketogenic diet, may be beneficial in the treatment of conditions associated with metabolic syndrome.
Case Report:
Here we present a case of a patient with metabolic syndrome successfully treated with the paleolithic ketogenic diet. While on the diet the patient was able to discontinue eight medicines, lost weight, showed a continuous improvement in glucose parameters, and her blood pressure normalized. Currently, the patient is on the paleolithic ketogenic diet for 22 months, free of symptoms and side effects.
Conclusion:
We conclude that the paleolithic ketogenic diet was safe, feasible, and effective in the treatment of this patient with metabolic syndrome.
Keywords: Paleolithic ketogenic diet, paleolithic diet, metabolic syndrome, hypertension, diabetes, obesity
INTRODUCTION
Obesity, type 2 diabetes, and hypertension represent a major health problem. These conditions are components of the metabolic syndrome affecting every fifth adult worldwide [1]. Although it is now acknowledged that type 2 diabetes and hypertension mostly result from lifestyle factors [2] medical treatment continues to rely on drugs. Symptoms of the metabolic syndrome typically show up in mid-life but the number of co-morbidities are increasing through later years. Typically symptoms are controlled with an increasing number of drugs. In parallel side effects are also increasing and are usually controlled with additional medications. It is a vicious circle. Currently, a major proportion of the elderly in the western world is overmedicated [3]. In sharp contrast with this diseases of civilization are virtually absent in contemporary hunter-gatherer societies [4]. It is suggested that chronic diseases of civilization result from an evolutionary mismatch between our ancient and current diets [5]. It was also suggested that a return to an evolutionary adapted diet may be beneficial for health [5]. The paleolithic diet has previously been shown to confer metabolic benefits is healthy as well as in patients with metabolic syndrome [6-10]. Voegtlin [11], the first proponent of the human evolutionary diet, suggested an animal meat-based diet as being evolutionary adapted. Recently we reported successful treatment of patients with epilepsy [12] and type 1 diabetes [13] with the paleolithic ketogenic diet. The diet we refer to as the paleolithic ketogenic diet is close to the meat-fat-based diet originally proposed by Voegtlin [11]. Herein, we report on a patient with obesity, type 2 diabetes, and hypertension whose excessive medication could be discontinued and clinical parameters associated with the metabolic syndrome markedly improved.
CASE REPORT
Previous medical history
The patient’s previous medical history included gall bladder surgery in 1987 due to choledocholithiasis and chronic cholecystitis. Hyperglycemia and impaired glucose tolerance were first demonstrated on 24 Feb 2004. Due to bloody stool, Weber test was performed on 25 Aug 2006 which showed positivity. Therefore colonoscopy was performed on 19 Sep 2006 which indicated a 2-cm polyp in the sigmoid colon. Irrigoscopy performed on 25 Sep 2006 confirmed the above-mentioned polyp and also indicated dilation of the colon as well as sigmoid diverticulosis. The polyp was removed on 6 Nov 2006. Histopathology from this specimen showed tubulovillous adenocarcinoma in polyp (Grade 1). Resection margins were negative. Gastroscopy performed on 21 Sep 2006 indicated reflux oesophagitis and erosive gastritis. Gastroscopy follow-up, three years later, on 26 Jan 2009 indicated reflux oesophagitis but no evidence of gastritis. A next gastroscopy follow-up on 26 Jan 2011, showed reflux oesophagitis and a 5-mm gastric polyp which was removed. Histopathology from this sample showed no abnormalities. A subsequent gastroscopy performed on 14 March 2013 showed reflux oesophagitis. Colonoscopy follow-up on 26 Jan 2007 demonstrated dilation of colon. Subsequent colonoscopy examinations on 27 Aug 2007, 25 Aug 2008, 31 Aug 2009, and 15 Apr 2013 were able to examine the colon until the transversus lienalis and showed no alterations. A CT colonography on 27 Apr 2011 was negative too.
On 10 Dec 2009, she experienced pressing pain behind the sternum. Echocardiography on 14 Dec 2009 showed impaired left ventricular diastolic function as well as aortic and mitral insufficiency.
A routine ophthalmological examination on 01 Jun 2006 showed crossing phenomenon and hyperaemic macula, ocular signs of hypertonia and diabetes. Follow-up ophthalmology examination on 20 May 2009 and on 21 May 2010 showed angiopathy while follow-up examinations on 18 May 2012 and 30 July 2013 indicated angiopathy as well as retinopathy.
Medications
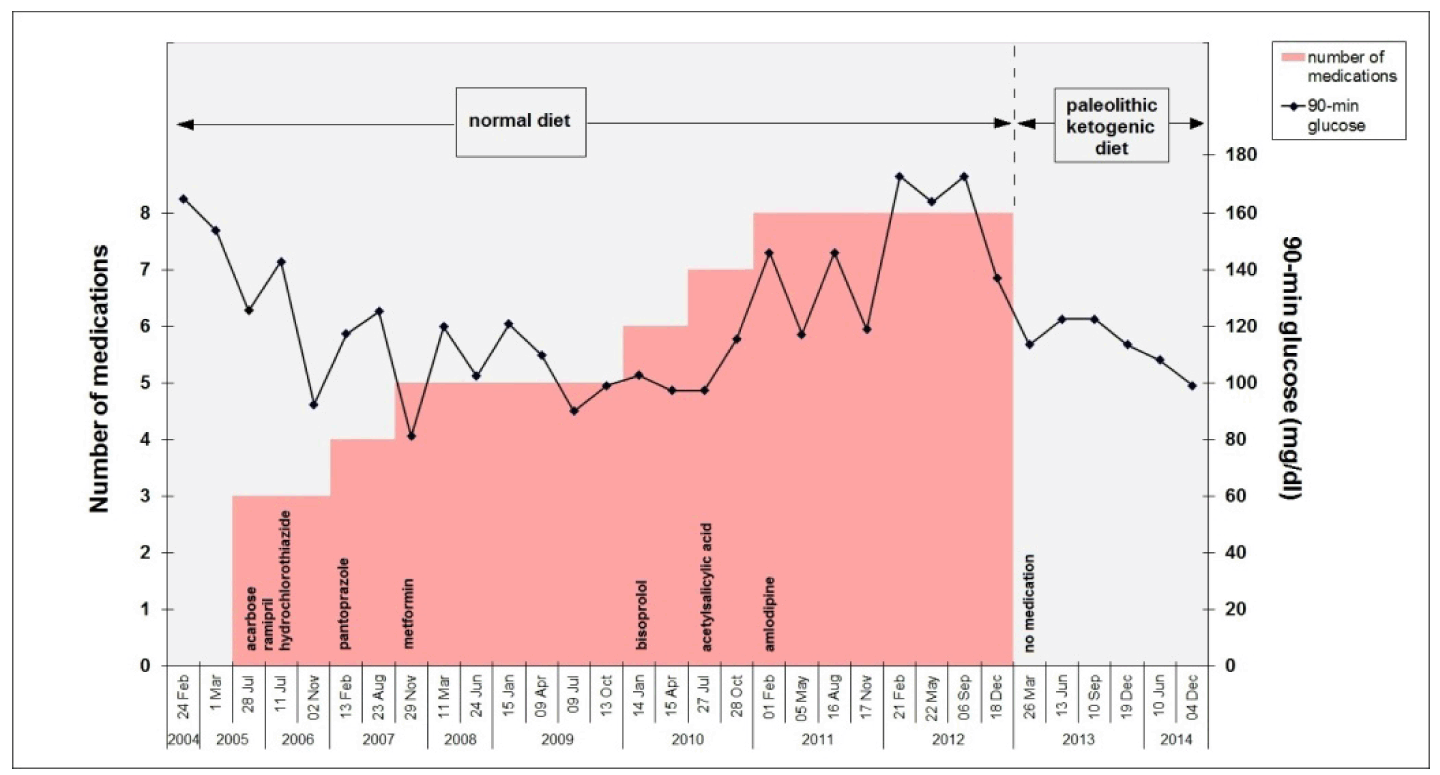
Due to elevated blood glucose parameters from 01 Mar 2005 on the patient was treated with acarbose, ramipril, and hydrochlorothiazide. On 02 Nov 2006 pantoprazole was added because of reflux oesophagitis revealed by gastroscopy. Due to increases in blood glucose from 23 Aug 2007, she was also taking metformin. On 14 Dec 2009 bisoprolol was added because of high blood pressure. Following the cardiological event acetylsalicylic acid was prescribed on 15 Apr 2010. From 28 Oct 2010, she was prescribed amlodipine due to high blood pressure. The number and the names (active substance) of the medications taken through the course of the disease and the associated 90-min glucose are indicated in Figure1.
Paleolithic ketogenic diet
We first met the 65-year-old patient on 30 Jan 2013. She was overweight (BMI=37.1; height: 160 cm; weight: 95kg), had high blood sugar, and frequent high blood pressure spikes despite antidiabetic and antihypertensive medication. At this time her systolic blood pressure was between 130 and 160 Hgmm and diastolic blood pressure between 70 and 85 Hgmm. Her fasting glucose level was between 144 and 162 mg/dl. Altogether she was taking eight medicines. The patient was motivated in weight loss and in the reduction of her medication. She was advised to start the paleolithic ketogenic diet. She was suggested a diet consisting of at least 70% animal-based food with a fat:protein ratio of at least 2:1. Fat and red meats were preferred over lean meats. Offals were encouraged to ensure adequate intake of vitamins. No more than 30% of the diet was suggested as plant-derived food including root vegetables and small amounts of fruit. Dairy, cereals, grains, legumes, solanaceous vegetables, plant oils (including coconut oil), artificial sweeteners, and foods with additives were not allowed. In addition to the paleolithic ketogenic diet she was taking 2000 IU of vitamin D3 for four months then it was stopped. No other vitamin or mineral supplements were used. Typical foods the patient was eating include broth, stew, fried bacon, beef steak, stewed calf liver, braised pork marrow, greaves. Vegetables consumed as garnish were limited and typically included root vegetables, onion and cabbage.
Upon diet commencement (on the third day of the diet) all medications were stopped promptly except for bisoprolol which was discontinued within two weeks. The patient was controlled tightly during the first weeks of the diet. In case of high blood pressure, she was advised to take captopril, a short-acting antihypertensive.
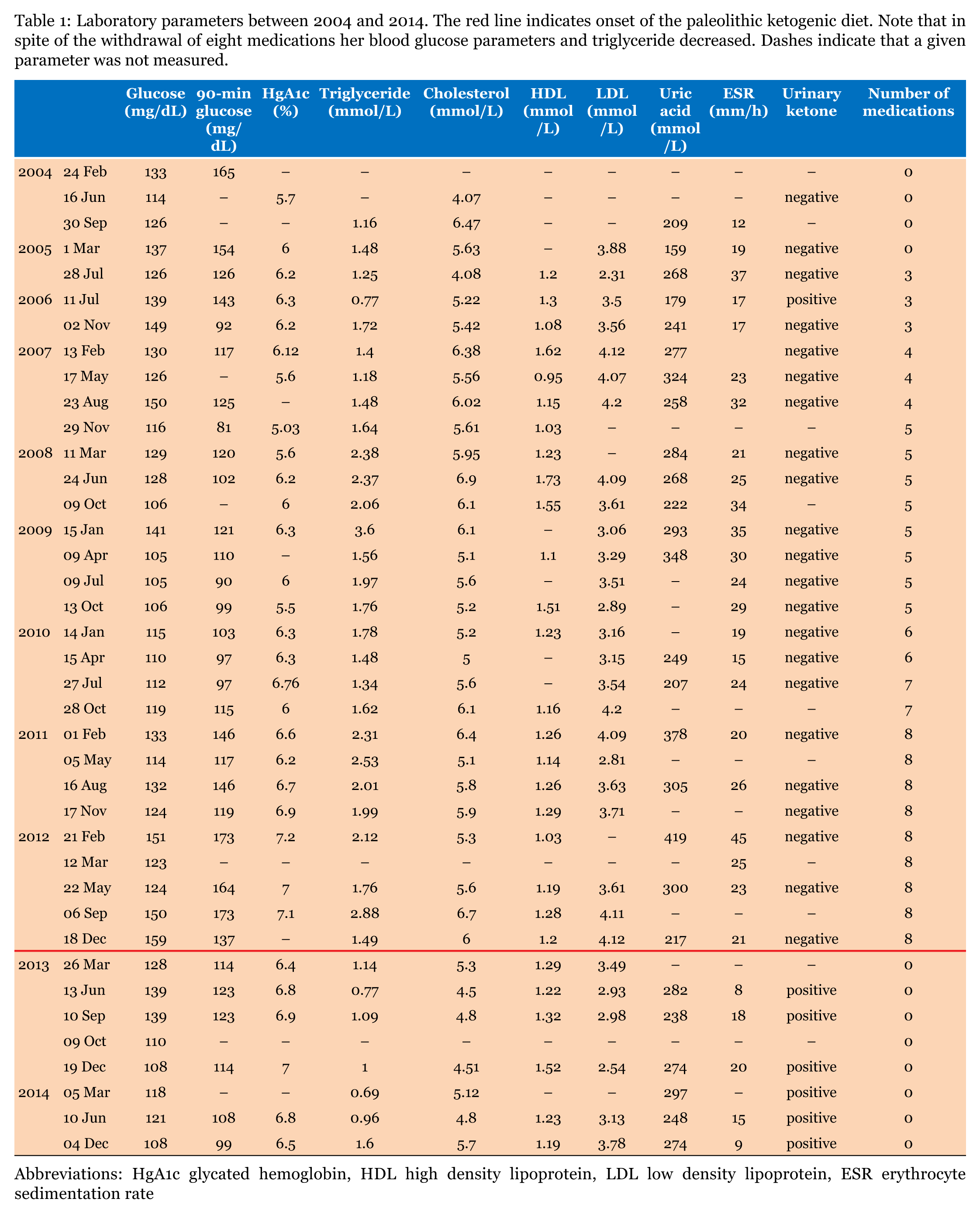
Laboratory workup was performed regularly (eight times during 22 months on the diet) in order to control adherence to the diet and to give feedback to the patient (Table 1). All urinary analyses were positive for ketones. While on the paleolithic ketogenic diet blood glucose level, 90-min glucose on the glucose tolerance test, HgA1c, and total cholesterol levels decreased as compared to previous measurements. Triglyceride levels also dropped markedly as well as inflammatory markers including erythrocyte sedimentation rate. A statistical analysis (t-test) comparing laboratory measures during the two years of the paleolithic ketogenic diet and during the previous nine years on a normal diet revealed a significant decrease for HgA1c (p=0.02), cholesterol (p=0.01), and triglyceride (p=0.003).
Typically the patient had two meals a day. She tracked glucose levels daily both preprandially and postprandially before and after the first meal of the day.
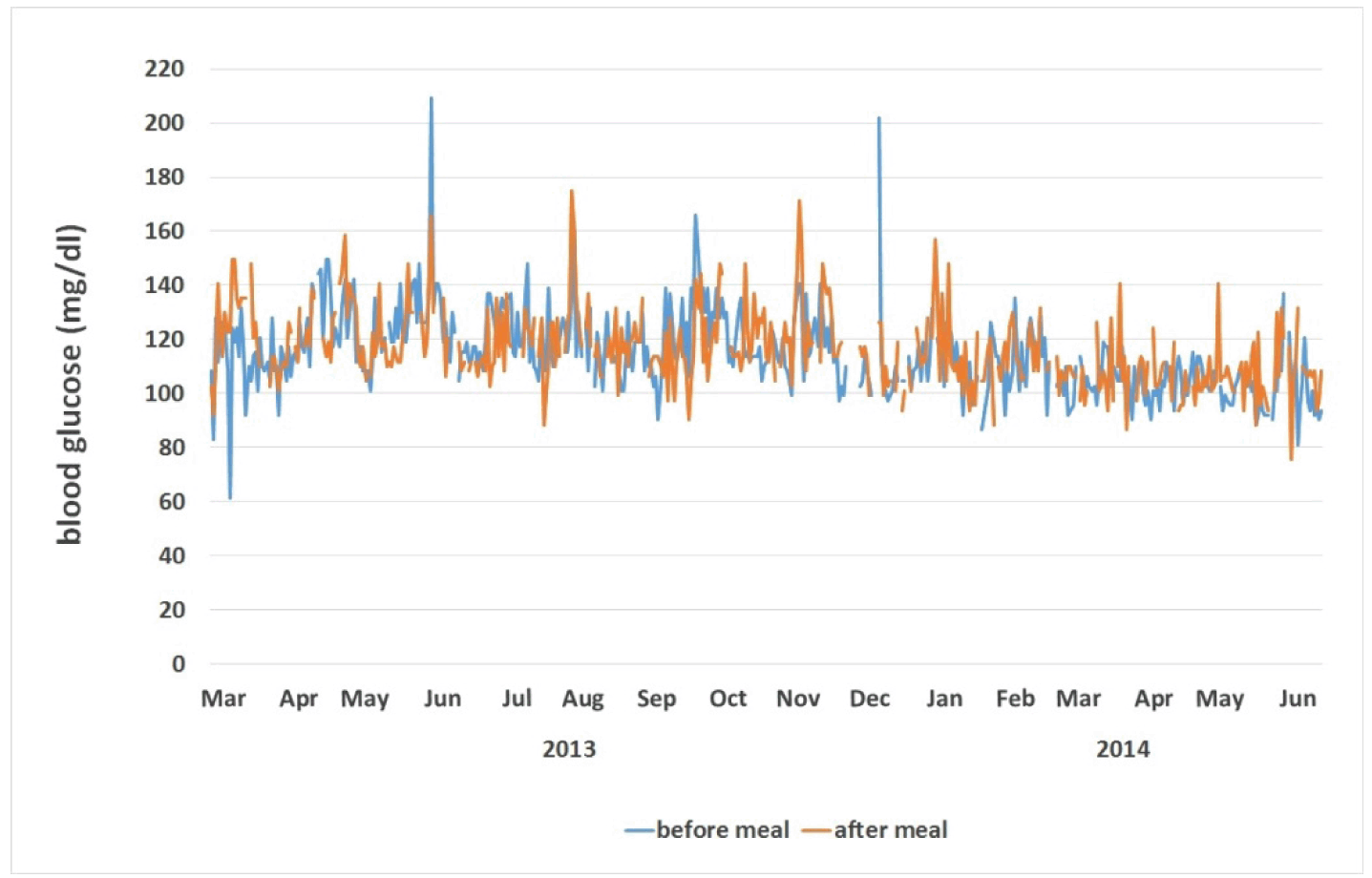
The patient reported to strictly adhere to the diet insofar not consuming non-paleolithic food at all. At the same time, she admitted having some difficulties with fruit restriction and reported that her spikes in blood sugar (Figure 2) and blood pressure to be associated with these events of excess fruit intake. Nevertheless, home monitoring of glucose showed a clear decreasing trend both preprandially and postprandially between February 2013 and June 2014 (Figure 2). Then due to the normalization of blood glucose, she measured blood glucose levels only occasionally. While on the diet she also reported a decreasing tendency in the frequency of high blood pressure spikes. At the time of writing the manuscript, she has had no high blood pressure spike for six months. Despite no vitamin D supplementation, her wintertime vitamin D level (on 05 March 2014) was in the normal range (85 nmol/l). The patient did not perform exercise while on the paleolithic diet.
Currently, she is on the diet for 22 months. While on the diet her weight changed from 95 kg to 81 kg and she is still losing weight. Her BMI changed from 37.1 to 31.6. She reports increased physical fitness and being free of symptoms.
The patient gave written informed consent for the publication of her case.
DISCUSSION
Recent clinical studies show that low-carbohydrate diets including the paleolithic diet are beneficial in conditions associated with the metabolic syndrome [6-10]. In the current medical practice, patients with metabolic syndrome are generally treated with numerous drugs. Yet studies available on the paleolithic diet do not give clues on how to deal with preexisting medications when shifting toward the paleolithic diet. Our experience indicates that upon the shift toward the paleolithic ketogenic diet most drugs become unnecessary and should be discontinued [14].
Here we analyzed the past medical history of a patient with metabolic syndrome to reveal how her medication might have contributed to the worsening of her disease and how the disease was influenced by the paleolithic ketogenic diet.
Our case represents a typical disease career of a patient with metabolic syndrome. Her medical history included elevated glucose parameters initially controlled with oral antidiabetics in 2005. Then with the emergence of new diagnostic findings pantoprazole was added. Two years later metformin was added to support glucose metabolism. Nevertheless, glucose control deteriorated again in 2011 following the addition of three new drugs. These included bisoprolol, acetylsalicylic acid, and amlodipine. Bisoprolol and amlodipine, which belong to beta-blockers and calcium channel blocker type antihypertensives, respectively, are known for their effect to adversely affect glucose metabolism [15, 16]. Glucose parameters further deteriorated in 2012.
Current guidelines first advise lifestyle changes and exercise to treat metabolic syndrome and to induce weight loss [1]. Yet this dietary advice usually remain without effect [17]. Also, overweight people are unable to exert considerable physical activity. Therefore patients are prescribed medications. A main problem is that in current medical practice each component of the metabolic syndrome is treated separately even though targeting one symptom by a drug may worsen another symptom also associated with the metabolic syndrome. Therefore the number of drugs, as well as side effects, are increasing.
Our patient was overweight and was taking eight medicines. When shifting toward the paleolithic ketogenic diet she was able to discontinue all medications. Her weight begin to decrease along with improving glucose parameters and lowered blood pressure. Our experience with patients on the paleolithic ketogenic diet indicates that the use of antihypertensive drugs hinders the normalization of glucose levels and weight loss [14]. Also, antihypertensive drugs become unnecessary since the paleolithic ketogenic diet efficiently lowers high blood pressure. In this case, antihypertensive drugs could be discontinued because the patient had no arteriosclerosis. In those cases with arteriosclerosis antihypertensives may be discontinued only within a longer time period. The blood pressure-lowering effect of the paleolithic ketogenic diet is due to the fact that the paleolithic ketogenic diet limits those food components which result in elevated blood pressure. These components mainly include fruits and foods with added fructose. A decrease of blood pressure was also reported in previous studies with the paleolithic diet [6, 8]. Our experience with patients with hypertension indicates that as compared to the paleolithic diet which does not limit fruits and vegetables, the paleolithic ketogenic diet more efficiently normalizes blood pressure. Given that in the paleolithic ketogenic diet carbohydrate intake is strongly limited less insulin is required for normoglycemia and therefore oral antidiabetics become unnecessary.
While on the paleolithic ketogenic diet home monitoring of glucose in our patient showed a decreasing tendency both preprandially and postprandially. Laboratory measurements also showed a decreasing tendency in glucose parameters and triglyceride normalized too. Total cholesterol and LDL cholesterol tended to decrease while HDL cholesterol remained relatively unchanged. Uric acid remained in the normal range while on the paleolithic ketogenic diet. These laboratory parameters are similar to those in our two previous cases on the paleolithic ketogenic diet [12, 13]. All six urinary tests were positive for ketones indicating a good adherence to the diet. The patient admitted to occasionally exceed the advised limit for fruit. She also linked excessed fruit intake to high blood pressure spikes which are in accordance with the literature data showing high blood pressure to be associated with fructose [18]. Nevertheless, our patient reported a decreasing tendency of blood pressure across the 22 months.
Those patients who underwent gall bladder surgery are advised against eating fatty foods and the ketogenic diet too. Our patient, however, reported no gastrointestinal side effects while on the paleolithic ketogenic diet. Of note, her winter-time vitamin D level was normal in spite of no vitamin D supplementation indicating that a regular intake of offal, animal fat, and meat may ensure normal vitamin D status. Also, no signs of vitamin or mineral deficiency emerged despite the lack of supplementation.
Currently, the patient is on the paleolithic ketogenic diet for 22 months. No side effects emerged and she is free of symptoms. She is resolute to continue the diet.
CONCLUSION
The paleolithic ketogenic diet proved to be a safe, feasible, and effective therapy in the case of this patient with metabolic syndrome. Medications could be discontinued and components of the metabolic syndrome improved continuously. We used the paleolithic ketogenic diet in a patient without a gall bladder indicating that, contrary to the widely held notion, this organ is not a prerequisite for maintaining the diet rich in animal fat.
Neither vitamin nor other supplements were used indicating the effectiveness of the paleolithic ketogenic diet as a sole therapy.
CONFLICT OF INTEREST
The authors declare no conflict of interest.
REFERENCES
1. International Diabetes Federation: The IDF consensus worldwide definition of the metabolic syndrome. Available at: http://www.idf.org/metabolic-syndrome Accessed December 8, 2014.
2. Perez-Pastor EM, Metcalf BS, Hosking J, Jeffery AN, Voss LD, Wilkin TJ. Assortative weight gain in mother-daughter and father-son pairs: an emerging source of childhood obesity. Longitudinal study of trios (EarlyBird 43). Int J Obes (Lond). 2009;33(7):727-35.
3. Hofer-Dückelmann C. Gender and polypharmacotherapy in the elderly: a clinical challange. In: Sex and Gender Differences in Pharmacology (Ed: Regitz-Zagrosek V) 2002. p. 169-182.
4. Lindeberg S. Food and western disease: health and nutrition from an evolutionary perspective. Chichester: Wiley-Blackwell; 2009.
5. Cordain L. The paleo diet: lose weight and get healthy by eating the food you were designed to eat. New York: Wiley; 2002.
6. Österdahl M, Kocturk T, Koochek A, Wändell PE. Effects of a short-term intervention with a paleolithic diet in healthy volunteers. Eur J Clin Nutr. 2008;62(5):682–5.
7. Jönsson T, Granfeldt Y, Ahrén B, Branell UC, Pålsson G, Hansson A, Söderström M, Lindeberg S. Beneficial effects of a Paleolithic diet on cardiovascular risk factors in type 2 diabetes: a randomized cross-over pilot study. Cardiovasc Diabetol. 2009;8:35.
8. Frassetto LA, Schloetter M, Mietus-Synder M, Morris RC Jr, Sebastian A. Metabolic and physiologic improvements from consuming a paleolithic, hunter-gatherer type diet. Eur J Clin Nutr. 2009;63(8):947–55.
9. Mellberg C, Sandberg S, Ryberg M, Eriksson M, Brage S, Larsson C, Olsson T, Lindahl B. Long-term effects of a Palaeolithic-type diet in obese postmenopausal women: a 2-year randomized trial. Eur J Clin Nutr. 2014 Mar;68(3):350-7.
10. Boers I, Muskiet FA, Berkelaar E, Schut E, Penders R, Hoenderdos K, Wichers HJ, Jong MC. Favourable effects of consuming a Palaeolithic-type diet on characteristics of the metabolic syndrome: a randomized controlled pilot-study. Lipids Health Dis. 2014;13:160.
11. Voegtlin WL. The stone age diet: based on in-depth studies of human ecology and the diet of man. New York: Vantage Press; 1975.
12. Clemens Z, Kelemen A, Fogarasi A, Tóth C. Childhood Absence Epilepsy Successfully Treated with the Paleolithic Ketogenic Diet. Neurology and Therapy 2013;2(1-2):71–6.
13. Tóth C, Clemens Z. Type 1 diabetes mellitus successfully managed with the paleolithic ketogenic diet. Int J Case Rep Images 2014;5(10):699–703.
14. Tóth C. Paleolithic medicine (Paleolit orvoslás). Budapest: Jaffa; 2012.
15. Blackburn DF, Wilson TW. Antihypertensive medications and blood sugar: theories and implications. Can J Cardiol. 2006;22(3):229-33.
16. Levine M, Boyer EW, Pozner CN, Geib AJ, Thomsen T, Mick N, Thomas SH. Assessment of hyperglycemia after calcium channel blocker overdoses involving diltiazem or verapamil. Crit Care Med. 2007;35(9):2071-5.
17. Accurso A, Bernstein RK, Dahlqvist A, Draznin B, Feinman RD, Fine EJ et al. Dietary carbohydrate restriction in type 2 diabetes mellitus and metabolic syndrome: time for a critical appraisal. Nutr Metab (Lond). 2008;5:9.
18. Madero M, Perez-Pozo SE, Jalal D, Johnson RJ, Sánchez-Lozada LG. Dietary fructose and hypertension. Curr Hypertens Rep. 2011;13(1):29-35.
 Rehabilitáció csak online elérhető
Rehabilitáció csak online elérhető
 E-mail: paleomedicina@gmail.com
E-mail: paleomedicina@gmail.com


